Is diabetes reversal true?
New research suggests that many people with Type 2 diabetes can improve insulin resistance and blood sugar levels. They can do this through targeted lifestyle and medical strategies.
Scientific studies now show that substantial weight loss, especially in the early stages of the disease, can significantly improve metabolic function and even lead to periods of remission.
The word “reversal” may sound absolute. But evidence shows that improving key metabolic problems, like excess fat and insulin resistance, helps the body control blood sugar better.
Understanding what the science truly supports can help individuals make informed, realistic decisions about their long-term health and diabetes management.
What Does Current Research Say About Diabetes Reversal in Type 2 Diabetes?

Current studies show that many people with Type 2 diabetes can reverse the disease. This happens when factors like excess liver fat, poor beta-cell function, and low insulin production improve a lot.
Research highlights that substantial weight loss, especially early in the disease, can restore healthier blood sugar levels and enhance overall glycemic control.
Trials using low-calorie diets, structured lifestyle changes, and targeted approaches like a ketogenic diet show that reducing body fat helps. Improving physical activity also supports returning to normal glucose control.
Remission happens more often in Type 2 diabetes than in Type 1 or gestational diabetes. Scientists agree that with ongoing effort, people can improve a lot and sometimes reach remission.
Key Research Insights
- Weight loss of 10–15 kg has been shown to significantly reduce liver fat, improve insulin sensitivity, and help restore beta-cell and beta-cell function, a major driver of remission.
- Low-calorie diets in clinical trials have led to rapid improvements in blood sugar levels and helped many individuals achieve remission in Type 2 diabetes.
- Structured lifestyle interventions combining nutrition, physical activity, and long-term support improve glycemic control and increase the chances of sustained remission.
- A ketogenic diet may lower blood sugar levels quickly by reducing carbohydrate intake and improving metabolic flexibility, though long-term results vary.
- Improvements in insulin production often occur when fat around the pancreas and liver is reduced, allowing the body to regulate blood glucose more effectively.
- Remission outcomes in Type 1 diabetes and gestational diabetes are more limited, as the underlying mechanisms differ from Type 2 diabetes.
- Early diagnosis increases the likelihood of remission because metabolic damage and beta-cell loss are less advanced.
How Does Weight Loss Influence Diabetes Reversal and Long-Term Diabetes Remission?

Weight loss plays a central role in diabetes reversal and long-term remission, particularly in individuals with Type 2 diabetes.
Scientific evidence shows that reducing extra fat, especially in the liver and around the pancreas, greatly improves how the body manages glucose and insulin.
Major clinical trials show that even moderate weight loss can restore metabolic balance. This helps control blood sugar better and makes remission possible for many people.
1. Why Weight Loss Is a Key Driver of Diabetes Reversal
In individuals with Type 2 diabetes, excess body fat disrupts the body's ability to effectively use insulin, which results in higher blood levels.
Scientific studies have demonstrated that reducing fat accumulation specifically in the liver and pancreas can significantly help restore the body's insulin sensitivity, allowing for improved management of glucose levels.
Key Points
- Weight loss reduces fat in the liver, improving metabolic function and lowering blood glucose.
- Losing significant weight can restore pancreatic insulin secretion, helping support natural glucose regulation.
- Clinical trials like DiRECT show that weight loss is the strongest predictor of diabetes reversal.
2. How Weight Loss Restores Insulin Sensitivity
Weight loss improves insulin sensitivity because it directly reduces fat stored in vital organs and improves overall metabolic health.
Key Points
- Lower liver fat improves how the liver responds to insulin, reducing excess glucose production.
- Reduced body fat improves muscle glucose uptake, further enhancing glycemic control.
- Improved insulin sensitivity helps maintain normal blood glucose levels over the long term.
3. The Role of Diet: Nutrition, Low-Calorie Plans, and Ketogenic Approaches
Different nutrition strategies support weight loss and metabolic improvements.
Key Points
- Low-calorie diets used in clinical trials can rapidly lower glucose levels and reduce organ fat.
- A ketogenic diet may help reduce blood glucose by minimizing carbohydrate intake and improving insulin sensitivity.
- Sustainable nutrition changes are essential for maintaining remission after initial weight loss.
4. Physical Activity and Its Impact on Remission
Regular physical activity enhances the benefits of weight loss by improving insulin sensitivity and supporting metabolic health.
Key Points
- Exercise increases muscle glucose uptake, lowering blood glucose naturally.
- Physical activity helps maintain long-term weight stability and prevents relapse.
- Combined with diet, exercise significantly improves the chances of diabetes reversal.
5. What Clinical Trials Reveal About Long-Term Remission
Major clinical trials in Type 2 diabetes consistently show that weight loss is the most reliable predictor of remission.
Key Points
- Weight loss of 10–15 kg has doubled remission rates in multiple studies.
- Individuals who maintain long-term weight reduction have the highest chances of preserving glycemic control.
- Early intervention improves outcomes, especially in people with recent diagnoses.
6. How Weight Loss Impacts Prediabetes and Type 1 Diabetes
The effects of weight loss differ across diabetes types:
Prediabetes
- Weight loss dramatically reduces progression to Type 2 diabetes.
- Improved insulin sensitivity often normalizes blood glucose levels.
Type 1 Diabetes
- Weight loss does not cause reversal, but can improve overall metabolic health.
- Better weight management helps optimize insulin dosing and improve day-to-day glycemic control.
7. Medications That Support Weight-Loss-Driven Reversal
Certain medications offer metabolic benefits that complement weight loss.
Key Points
- SGLT2 inhibitors help lower blood glucose and modestly support weight reduction.
- Combined with diet and physical activity, medication may accelerate reversal efforts in Type 2 diabetes.
Can Improving Blood Sugars and Blood Sugar Levels Lead to Diabetes Remission?
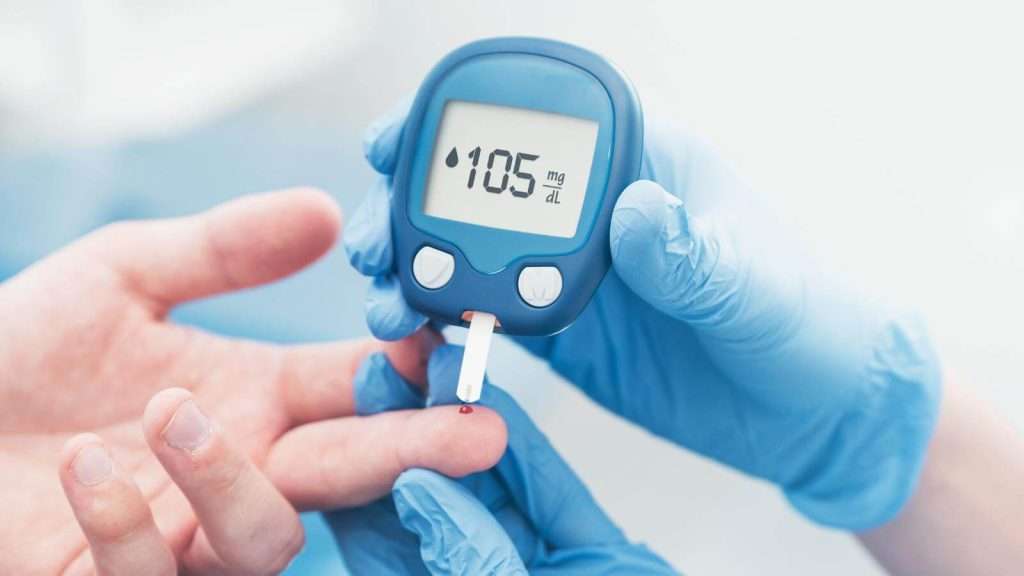
Maintaining optimal blood sugars and blood sugar levels is central to achieving diabetes remission, especially in Type 2 diabetes.
Research shows that early actions like better nutrition, exercise, weight loss, and specific medicines can restore blood sugar control. These actions can also improve pancreatic function. Some patients can reduce or stop their diabetes treatments.
Type 1 diabetes is mostly not reversible because the immune system destroys pancreatic beta cells. Prediabetes and early Type 2 diabetes have the best chance for remission when blood sugar levels are controlled.
1. Nutrition and Diet Strategies
Diet is a primary tool for controlling blood sugars and supporting remission.
Key Points
- Structured meal plans improve glycemic control and reduce the need for medications.
- Low-calorie diets and ketogenic diets can rapidly lower blood sugar levels and help restore pancreatic function.
- Consistent nutrition habits support long-term maintenance of diabetes remission.
2. Exercise and Physical Activity
Regular exercise enhances insulin sensitivity and helps normalize blood sugar levels.
Key Points
- Improves glucose uptake by muscles, lowering overall blood sugars.
- Supports weight management, which is strongly linked to diabetes remission.
- Works synergistically with diet to maintain long-term glycemic control.
3. Evidence from Clinical Trials: DiRECT Study
The DiRECT trial highlights how blood sugar improvements can lead to remission.
Key Points
- Participants with early Type 2 diabetes achieved remission after intensive weight loss and dietary intervention.
- Reductions in blood sugar levels corresponded with recovery of pancreatic function.
- Reinforces that early intervention is critical for sustained diabetes reversal.
4. Medications That Support Blood Sugar Control
Targeted medications can complement lifestyle strategies.
Key Points
- SGLT2 inhibitors help lower blood sugar levels and support weight loss.
- Some medications reduce the burden on the pancreas, preserving beta-cell function.
- Used strategically, medications can accelerate remission when combined with diet and exercise.
5. Differences in Diabetes Types
Type 1 Diabetes
- Optimizing blood sugars improves long-term outcomes but does not induce remission.
- Requires lifelong insulin therapy.
Prediabetes
- Early improvements in blood sugar levels can prevent progression to Type 2 diabetes.
- Lifestyle changes alone can often normalize glycemic control.
What Role Does Insulin Resistance Play in the Possibility of Diabetes Reversal?
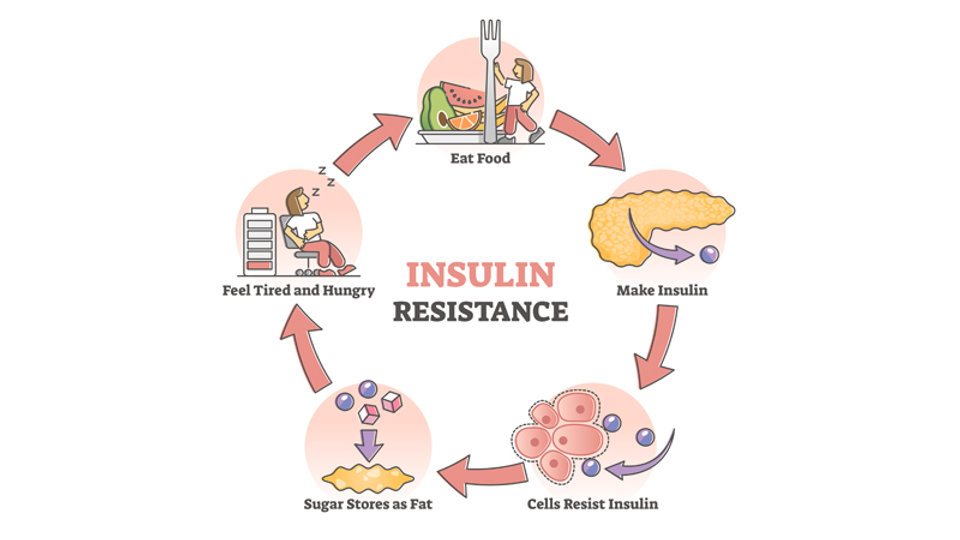
Insulin resistance is a key factor in the development of Type 2 diabetes and a major barrier to diabetes reversal.
When the body’s cells become less responsive to insulin, glycemic control worsens, leading to elevated blood sugar levels.
Research shows that reversing insulin resistance through lifestyle changes, structured exercise, and targeted nutritional strategies—such as a ketogenic diet—can significantly improve metabolic health and increase the likelihood of remission.
Early intervention in Prediabetes offers the greatest opportunity for restoring insulin sensitivity.
1. Understanding Insulin Resistance and Its Impact
Insulin resistance occurs when cells in muscles, fat, and the liver fail to respond effectively to insulin, resulting in higher blood glucose levels.
Key Points
- Insulin resistance is a primary driver of Prediabetes and Type 2 diabetes.
- Poor glycemic control caused by insulin resistance increases the risk of complications.
- Addressing insulin resistance is crucial for supporting diabetes reversal.
2. Lifestyle Changes to Improve Insulin Sensitivity
Adopting consistent lifestyle changes can dramatically reduce insulin resistance.
Key Points
- Structured exercise enhances insulin sensitivity by increasing glucose uptake in muscles.
- Incorporating healthy habits—like balanced meals and regular activity—improves glycemic control over time.
- Long-term adherence to these lifestyle changes is essential for sustaining diabetes remission.
3. Role of Diet and Ketogenic Approaches
Nutrition plays a vital role in reducing insulin resistance.
Key Points
- Ketogenic diets and low-carb approaches lower blood glucose and improve insulin sensitivity.
- Reducing dietary carbohydrates decreases the demand on the pancreas and supports better glycemic control.
- Combining diet with exercise and other lifestyle strategies maximizes the chance of diabetes reversal.
4. Evidence from Clinical Trials: DiRECT Study
The DiRECT trial provides compelling evidence linking insulin resistance reversal with diabetes remission.
Key Points
- Participants achieved remission through intensive weight loss and targeted lifestyle changes.
- Improvements in glycemic control were closely associated with reductions in insulin resistance.
- Early intervention in people with Prediabetes or recent-onset Type 2 diabetes was most effective.
5. Building Lasting Habits for Sustained Remission
Sustainable remission depends on embedding healthy habits into daily life.
Key Points
- Consistent exercise and mindful nutrition maintain insulin sensitivity.
- Creating a routine around lifestyle changes helps prevent relapse and preserves glycemic control.
- Long-term commitment is critical: remission is a marathon, not a sprint.
How Do Lifestyle Interventions Support Reversing Type 2 Diabetes?
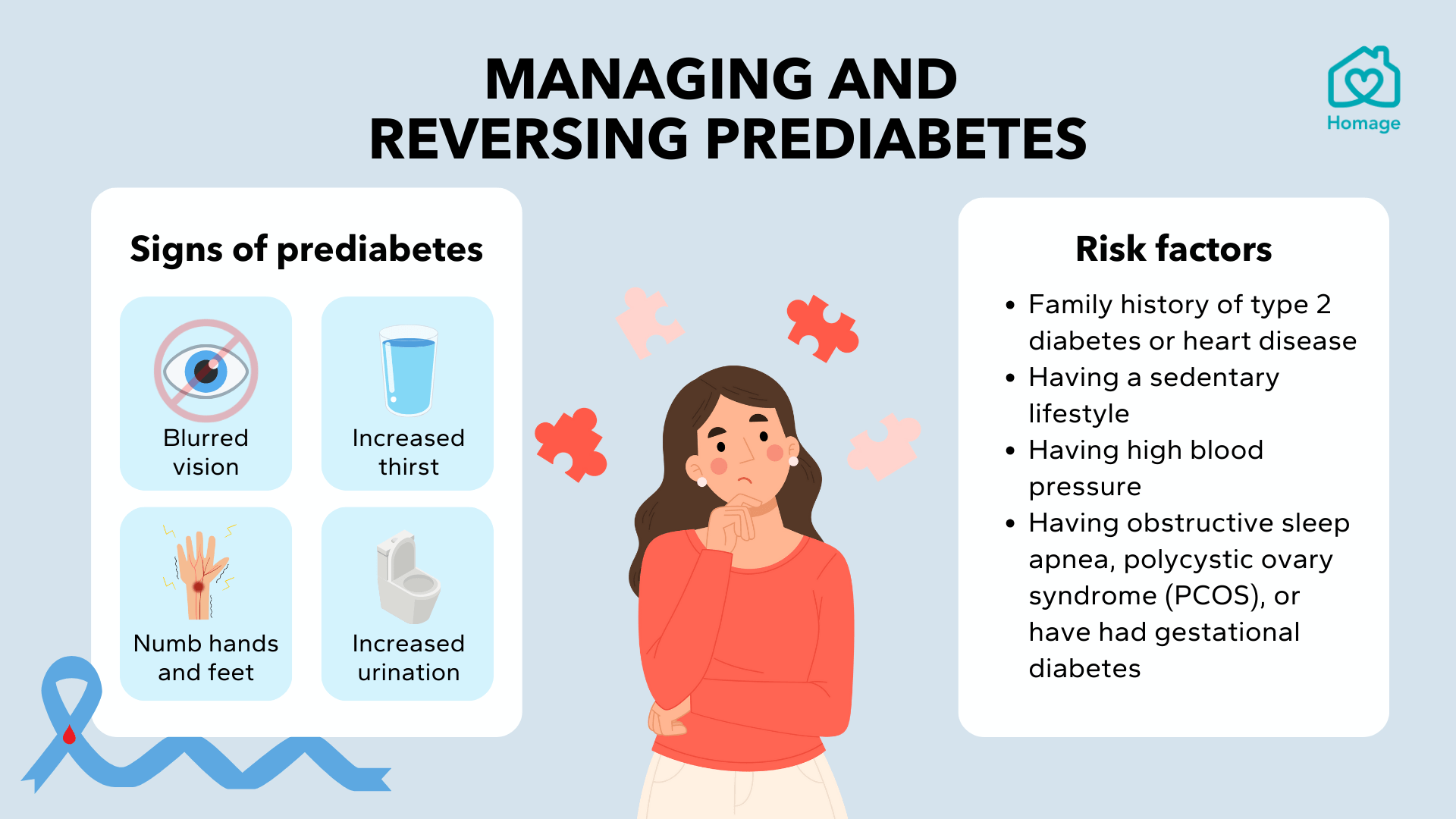
Lifestyle interventions are central to reversing Type 2 diabetes, especially when implemented early in the disease or during Prediabetes.
By combining structured nutrition, physical activity, and behavior modification, these interventions improve glycemic control, reduce insulin resistance, and sometimes lead to full remission.
Dietary approaches, including a ketogenic diet, are often incorporated as part of a comprehensive lifestyle strategy.
1. Early Intervention in Prediabetes
Targeting lifestyle factors during Prediabetes can prevent progression to Type 2 diabetes and even reverse early metabolic dysfunction.
Key Points
- Structured lifestyle interventions can normalize blood sugar levels and restore insulin sensitivity.
- Early adoption increases the likelihood of long-term diabetes reversal.
- Weight management and dietary changes are most effective before extensive pancreatic beta-cell dysfunction develops.
2. Nutrition Strategies in Lifestyle Interventions
Nutrition is a cornerstone of lifestyle-based reversal programs.
Key Points
- Calorie-controlled and low-carbohydrate diets, including a ketogenic diet, reduce blood glucose and improve glycemic control.
- Balanced meals that manage macronutrient intake help reduce insulin resistance.
- Nutrition-focused lifestyle interventions are often combined with behavior support for adherence and sustainability.
3. Physical Activity and Exercise
Incorporating regular exercise is essential for improving metabolism and supporting reversal.
Key Points
- Exercise improves glucose uptake in muscles, lowering blood sugar and insulin demand.
- Combined with nutrition, physical activity enhances the effectiveness of lifestyle interventions.
- Consistent activity supports long-term glycemic control and helps maintain weight loss.
4. Behavior and Habit Changes
Behavioral modifications make lifestyle changes sustainable.
Key Points
- Establishing consistent daily routines supports adherence to nutrition and exercise goals.
- Habit formation is critical to sustaining improvements in blood sugar levels.
- Lifestyle programs often include counseling or coaching to reinforce these habits.
5. Evidence Supporting Lifestyle Interventions
Clinical evidence confirms the effectiveness of lifestyle approaches for diabetes reversal.
Key Points
- Multiple studies demonstrate remission or near-normal glycemic control with comprehensive lifestyle interventions.
- Interventions are most successful when implemented early, particularly during Prediabetes or recent-onset Type 2 diabetes.
- A ketogenic diet is an effective dietary tool within these programs, especially for rapid reduction of blood glucose and weight management.
How Does Improving Insulin Production and Beta-Cell Function Affect Diabetes Remission?
Restoring insulin production and improving beta-cell function are critical steps toward achieving diabetes remission, particularly in Type 2 diabetes.
Beta cells in the pancreas are responsible for producing insulin, and their dysfunction leads to elevated blood glucose and poor glycaemic control.
Research shows that reducing liver and pancreas fat content, adopting low-carbohydrate ketogenic diets, and undergoing certain bariatric surgery procedures can help restore beta-cell responsiveness and support long-term remission.
1. The Role of Beta-Cell Function in Diabetes Remission
The health of pancreatic beta cells directly determines the body’s ability to produce insulin and regulate glucose levels.
Key Points
- Impaired beta-cell function leads to postprandial hyperglycemia and overall poor glycaemic control.
- Restoring beta-cell responsiveness improves insulin secretion and stabilizes blood glucose levels.
- Measurement of C-peptide levels can indicate beta-cell recovery in research and clinical settings.
2. Lifestyle and Nutritional Approaches
Certain natural therapies, low-carb diets, and nutritional ketosis strategies help relieve stress on beta cells and enhance insulin production.
Key Points
- Low-carbohydrate ketogenic diets reduce glucose spikes and improve insulin production efficiency.
- Intermittent fasting has been shown in some studies to improve beta-cell function and glycaemic control.
- Combined with lifestyle interventions, these approaches can lead to sustained improvements in blood sugar regulation.
3. Surgical and Pharmacological Interventions
Bariatric surgery, including gastric bypass and sleeve gastrectomy, can restore beta-cell function by reducing body weight and visceral fat.
Key Points
- Metabolic surgery has shown significant improvements in insulin production and remission rates in Type 2 diabetes.
- Glucagon-like peptide 1 (GLP-1) analogues and other glucose-lowering pharmacotherapy reduce beta-cell stress and enhance endogenous insulin secretion.
- Surgical interventions often lead to rapid improvements in glycaemic control before significant weight loss occurs.
4. Emerging Therapies: Stem Cells and Cell-Based Treatments
Research on stem cell therapy, islet cell transplantation, and reprogrammed stem cells aims to restore beta-cell function for patients who have lost significant insulin-producing capacity.
Key Points
- Islet cell transplantation can restore insulin production in select patients.
- Experimental stem cell therapies focus on regenerating beta cells for long-term diabetes reversal.
- While promising, these approaches are mostly experimental and primarily relevant for severe Type 1 diabetes or advanced Type 2 diabetes.
5. Supporting Long-Term Remission Through Monitoring and Maintenance
Maintaining beta-cell health is critical even after remission is achieved.
Key Points
- Continuous monitoring of blood glucose and glycaemic control helps prevent relapse.
- Combining dietary management, exercise, and medication routines ensures sustained beta-cell function.
- Early intervention and ongoing care, including guidance from sources like Diabetes Care and American Diabetes Association, improve long-term outcomes.
Is Diabetes Reversal True? What Research — and HealthyWayFit — Reveal

You may have heard conflicting ideas about Type 2 diabetes—some say it can’t be reversed, only managed. Others promise “quick fixes” or magic diets.
But what does science actually say?
Over the past decade, global research has shown a clear pattern:
For many people, Type 2 diabetes can be put into remission—meaning blood sugar levels return to the non-diabetic range without medications.
This isn’t about willpower. It’s about having the right system that addresses the root causes: nutrition, movement, metabolism, stress, and medical supervision.
That’s exactly where HealthyWayFit comes in.
What Makes HealthyWayFit Different?
1. Nutrition Based on Real Research — and Your Real Food
Studies show that sustainable, culturally appropriate diets help maintain long-term remission.
So instead of fad diets or complicated smoothie charts, we use your ghar ka khana—dal, roti, rice, idli, dosa, paneer, sabzi—and align it with metabolic needs.
No special cooking. No restrictions that don’t match Indian lifestyles.
2. Metabolic Exercise Proven to Improve Insulin Sensitivity
Research confirms that short, targeted muscle-activation routines significantly lower post-meal sugar levels.
Our 15–20 minute metabolic workouts require no gym or equipment and can be done by beginners at home.
3. Stress & Sleep Optimization — Backed by Science
High stress = high cortisol = higher sugar.
Evidence-based tools like one-minute breathing drills and sleep strategies help stabilize sugars even during hectic workdays.
4. Doctor-Led, Holistic Care
Every client works with a Senior MD Diabetologist plus certified lifestyle coaches.
This medical + lifestyle model follows global best-practice standards for safe diabetes remission.
5. Relentless Support & Accountability
Research shows that continuous guidance dramatically improves diabetes outcomes.
From weekly coaching to daily check-ins, travel and festival plans, you get support that adapts to your life—not the other way around.
What Results Can You Expect?
Most clients see positive changes—better energy, improved fasting sugars, lighter mornings—within 20–60 days.
Over 12 months, the focus shifts to long-term stabilization, because true diabetes remission must be sustainable, not temporary.
Who Is This Program For?
If you're a professional or entrepreneur with Type 2 diabetes and can dedicate 15–30 minutes a day, this system is built for you.
It’s not a shortcut. It’s a structured, evidence-based path to remission tailored to your food, family, and lifestyle.
Take the Next Step
Your journey starts with a personal consultation to understand your health history, challenges, and metabolic profile.
If you're a good fit, our team designs a custom Diabetes Reversal Plan built just for you.
Explore more at: healthywayfit
Book your consultation: calendly
Move beyond simply “managing” diabetes.
With the right system, support, and science, diabetes reversal is not just possible—it's achievable.
Frequently Asked Questions(FAQs)

1. What Does Research Show About Ketogenic Diets and Their Role in Reversing Type 2 Diabetes?
Research shows ketogenic diets reduce carbohydrate intake, lower blood glucose, improve insulin sensitivity, promote weight loss, and support glycemic control, making them a promising tool for Type 2 diabetes remission.
2. How Effective Are SGLT2 Inhibitors in Supporting Diabetes Remission?
SGLT2 inhibitors lower blood glucose by increasing urinary glucose excretion, modestly reduce weight, improve glycemic control, and complement lifestyle interventions, aiding Type 2 diabetes remission in combination therapies.
3. Is Diabetes Reversal Possible in Prediabetes and Gestational Diabetes?
Early interventions in Prediabetes and gestational diabetes using diet, exercise, and lifestyle modifications can normalize blood sugar, improve glycemic control, and sometimes achieve temporary diabetes reversal or remission.
4. What Does the Evidence Say About Diabetes Reversal for Type 1 Diabetes?
Due to autoimmune beta-cell destruction, Type 1 diabetes is generally irreversible. Research focuses on insulin therapy, glycemic control, and emerging treatments like stem cells or islet cell transplantation.
5. How Important Is Physical Activity for Improving Glycemic Control and Supporting Remission?
Regular physical activity improves insulin sensitivity, lowers blood glucose, promotes weight loss, enhances glycemic control, and is essential for sustaining Type 2 diabetes remission when combined with diet and lifestyle changes.
Conclusion
Current scientific research makes one thing clear: for many people with Type 2 diabetes, remission is possible when the right metabolic factors are addressed early and consistently.
Sustainable nutrition, targeted exercise, stress management, and medical supervision all work together to restore insulin sensitivity, improve beta-cell function, and stabilize blood sugar levels.
HealthyWayFit’s holistic, evidence-based approach brings these elements into a structured system designed for real Indian lifestyles.
With personalized guidance and ongoing support, individuals can move beyond short-term control toward long-term metabolic health—and for many, achieve true diabetes remission.

