Diabetes reversal particularly for type 2 diabetes is not a quick fix or a permanent cure. Instead, it is a clinically observed state in which blood sugar levels return to a non-diabetic range and remain stable without the need for glucose-lowering medication, as long as healthy lifestyle changes are maintained.
Growing research confirms that improving insulin sensitivity, reducing insulin resistance, lowering excess visceral fat, and restoring normal glucose metabolism are central to this process.
Studies now show that type 2 diabetes is driven more by metabolic dysfunction than by irreversible damage. By targeting root causes such as poor diet quality, excess calorie intake, physical inactivity, chronic inflammation, stress, and disrupted sleep, many individuals can significantly reduce blood sugar levels and achieve long-term diabetes remission.
Evidence-based strategies including balanced nutrition, controlled carbohydrate intake, weight loss, regular physical activity, and improved lifestyle habits play a critical role in supporting lasting results.
This article breaks down 9 important research-backed facts that explain how diabetes reversal really works, what makes it sustainable, and why consistency matters more than extreme interventions.
How does diabetes reversal really work, and what does research reveal?
Diabetes reversal particularly for type 2 diabetes is not a cure, but a scientifically observed process in which blood sugar levels return to a non-diabetic range without the need for glucose-lowering medication, as long as supportive lifestyle changes are maintained. Research shows that this happens when the core metabolic disturbances driving diabetes are corrected.
Rather than focusing only on lowering blood glucose, diabetes reversal works by restoring insulin sensitivity, organ function, and metabolic flexibility. Below are 9 important facts backed by scientific research that explain how this process works in the body.
Fact 1: Diabetes Reversal Works by Reversing Insulin Resistance at the Cellular Level
Insulin resistance is the central defect in type 2 diabetes. Research shows that in insulin-resistant states, muscle, liver, and fat cells fail to respond adequately to insulin, preventing glucose from entering cells efficiently. As a result, glucose remains in the bloodstream, leading to chronically elevated blood sugar levels.
Diabetes reversal improves insulin signaling pathways inside cells. When insulin sensitivity improves, glucose transporters become more active, allowing glucose to be absorbed and used for energy. This reduces both fasting and post-meal blood sugar levels and lowers the demand placed on the pancreas to produce insulin.
Fact 2: Excess Fat in the Liver Is a Major Driver of High Blood Sugar
Scientific research has identified fatty liver as a key contributor to type 2 diabetes. When excess fat accumulates in the liver, it disrupts insulin’s ability to suppress glucose production. This causes the liver to release glucose into the bloodstream even when it is not needed.
Studies show that reducing liver fat significantly improves fasting blood glucose levels. This improvement often occurs early in the diabetes reversal process sometimes within weeks demonstrating that restoring liver insulin sensitivity is a critical mechanism behind improved glucose control.
Fact 3: Reducing Fat Around the Pancreas Improves Insulin Secretion
The pancreas plays a crucial role in regulating blood sugar by producing insulin. Research indicates that fat infiltration in and around the pancreas interferes with beta-cell function, impairing insulin secretion.
When pancreatic fat decreases, beta cells regain their ability to release insulin in response to glucose. This restoration of first-phase insulin response is a key biological marker observed in diabetes remission studies and helps normalize post-meal blood sugar levels.
Fact 4: Modest Weight Loss Produces Disproportionate Metabolic Benefits
Clinical trials consistently show that losing as little as 5–10% of body weight can lead to significant improvements in insulin sensitivity and glycemic control. Importantly, the metabolic benefits of weight loss extend beyond the number on the scale.
Research emphasizes that the loss of visceral fat, fat stored deep within the abdomen has a greater impact on diabetes reversal than overall weight loss. This type of fat is metabolically active and strongly associated with inflammation, insulin resistance, and glucose dysregulation.
Fact 5: Calorie Restriction Rapidly Lowers Blood Sugar Independent of Weight Loss
Scientific studies have demonstrated that calorie reduction can lower blood sugar levels before significant weight loss occurs. This rapid improvement is primarily due to reduced glucose output from the liver and improved hepatic insulin sensitivity.
This finding explains why blood sugar often improves within days or weeks of dietary intervention. It highlights that diabetes reversal begins with metabolic changes at the organ level, not simply long-term changes in body composition.
Fact 6: Dietary Composition Strongly Influences Insulin Sensitivity
Research shows that diet quality plays a major role in diabetes reversal. Diets emphasizing whole, minimally processed foods such as vegetables, fiber-rich carbohydrates, lean protein, and healthy fats improve insulin sensitivity and reduce glucose variability.
High fiber intake slows glucose absorption, reducing post-meal spikes, while adequate protein helps preserve lean muscle mass. Limiting refined carbohydrates and ultra-processed foods reduces chronic insulin demand, allowing insulin signaling pathways to recover over time.
Fact 7: Physical Activity Enhances Glucose Uptake Through Insulin-Independent Pathways
Exercise has a unique role in diabetes reversal because muscle contraction allows glucose to enter cells without insulin. Scientific studies show that both aerobic and resistance training increase glucose transporter activity in muscle tissue.
Regular physical activity also increases muscle mass, which improves overall glucose disposal capacity. Over time, this leads to improved insulin sensitivity, lower fasting glucose, and better long-term glycemic stability.
Fact 8: Chronic Inflammation Interferes with Insulin Signaling
Low-grade, chronic inflammation is now recognized as a key contributor to insulin resistance. Research indicates that inflammatory molecules disrupt insulin signaling pathways, making glucose regulation more difficult.
Lifestyle interventions associated with diabetes reversal such as improved nutrition, weight loss, better sleep quality, and stress reduction have been shown to reduce inflammatory markers. Lower inflammation improves insulin responsiveness and supports metabolic recovery.
Fact 9: Clinical Studies Confirm Diabetes Remission Is Biologically Possible
Large clinical studies have documented diabetes remission in individuals who achieved and maintained significant metabolic improvements. These studies show that normal blood sugar levels can persist for years when lifestyle changes are sustained.
Research also indicates that earlier intervention increases the likelihood of success. Individuals with shorter diabetes duration and better-preserved beta-cell function tend to experience more durable results, reinforcing the importance of timely metabolic intervention.
What does research say about diabetes reversal and insulin sensitivity?

Research clearly shows that diabetes reversal is fundamentally driven by improvements in insulin sensitivity, which refers to how effectively the body’s cells respond to insulin and regulate blood glucose.
In type 2 diabetes, insulin resistance develops in key tissues such as the liver, skeletal muscle, and adipose tissue, causing glucose to remain in the bloodstream instead of being taken up by cells.
Scientific studies demonstrate that when insulin sensitivity improves, these metabolic abnormalities begin to reverse, allowing blood sugar levels to return to a non-diabetic range in many individuals, especially when changes are made early and maintained consistently.
Improved insulin sensitivity reduces the demand placed on the pancreas to produce excess insulin. Research indicates that as cells respond better to insulin, glucose uptake becomes more efficient, fasting and post-meal blood sugar levels decline, and pancreatic beta-cell function is preserved.
These changes explain why many diabetes reversal interventions lead to rapid improvements in glycemic control, sometimes occurring before significant weight loss is visible.
Scientific evidence highlights the liver as a central organ in diabetes reversal. In insulin-resistant states, the liver continues to release glucose even when blood sugar levels are already elevated.
Research shows that improving liver insulin sensitivity often through calorie reduction and loss of liver fat significantly reduces hepatic glucose output, leading to lower fasting blood sugar levels. This liver-specific improvement is one of the earliest metabolic changes observed in successful diabetes reversal.
Muscle insulin sensitivity is equally important. Studies confirm that skeletal muscle is responsible for the majority of glucose disposal after meals, and insulin resistance in muscle tissue leads to prolonged post-meal glucose spikes.
When insulin sensitivity improves in muscle, glucose uptake and storage increase, stabilizing blood sugar levels throughout the day. This is why physical activity is consistently associated with improved insulin sensitivity in diabetes reversal research.
Excess visceral and ectopic fat plays a major role in impairing insulin action. Research shows that fat accumulation releases free fatty acids and inflammatory molecules that interfere with insulin signaling pathways.
When this fat is reduced, insulin receptors function more effectively, glucose transport improves, and overall insulin resistance decreases. Importantly, studies demonstrate that even modest fat loss can lead to significant improvements in insulin sensitivity and blood sugar control.
Chronic low-grade inflammation is another well-established contributor to insulin resistance. Scientific studies indicate that inflammation disrupts insulin signaling at the cellular level.
Lifestyle interventions linked to diabetes reversal such as dietary improvements, regular physical activity, adequate sleep, and stress reduction have been shown to lower inflammatory markers, further enhancing insulin sensitivity and metabolic health.
Long-term clinical trials confirm that insulin sensitivity can be partially or substantially restored, particularly in individuals with shorter diabetes duration. Research also shows that maintaining improved insulin sensitivity is essential for sustaining diabetes reversal, as a return to insulin-resistant behaviors often leads to relapse.
Key research-backed conclusions include:
- Insulin resistance is the primary metabolic defect in type 2 diabetes
- Improving insulin sensitivity directly lowers fasting and post-meal blood sugar
- Liver insulin sensitivity is critical for normalizing fasting glucose
- Muscle insulin sensitivity determines post-meal glucose control
- Reducing visceral and organ fat restores insulin signaling
- Calorie reduction can rapidly improve insulin sensitivity
- Lower inflammation supports better insulin action
- Sustained insulin sensitivity is necessary for long-term diabetes reversal
Overall, research consistently shows that diabetes reversal works by restoring insulin sensitivity across multiple organs, leading to improved glucose regulation and long-term metabolic stability.
How does reducing insulin resistance help reverse diabetes?
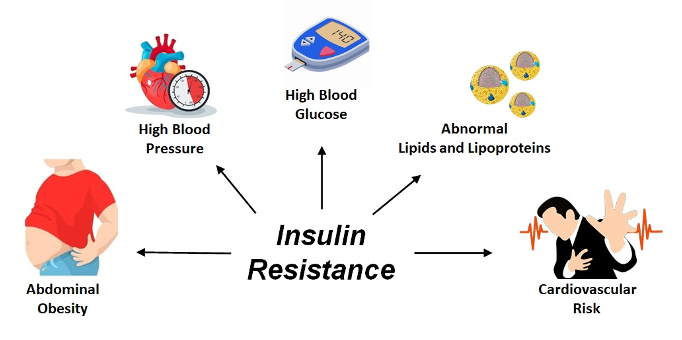
Reducing insulin resistance is the central biological mechanism behind successful diabetes reversal, particularly in type 2 diabetes. Insulin resistance occurs when the body’s cells mainly in the liver, skeletal muscles, and adipose tissue fail to respond properly to insulin.
This prevents glucose from entering cells efficiently and causes blood sugar to remain elevated. Research shows that when insulin resistance is progressively reduced, glucose metabolism normalizes, insulin demand decreases, and long-term blood sugar control becomes possible without medication in many individuals.
1) Insulin Resistance Is the Primary Driver of Type 2 Diabetes Progression
Type 2 diabetes does not begin with high blood sugar alone it begins with insulin resistance that develops gradually over years. As insulin resistance increases, the pancreas compensates by producing larger amounts of insulin to maintain normal glucose levels.
This chronic overproduction eventually overwhelms pancreatic beta cells, leading to persistent hyperglycemia and diabetes progression.
When insulin resistance is reduced:
- Cells regain their ability to respond to insulin
- Blood glucose moves efficiently into tissues
- The pancreas is relieved from constant overwork
Research confirms that addressing insulin resistance at its root can halt and even reverse the progression of type 2 diabetes.
2) Improved Insulin Sensitivity Restores Cellular Glucose Transport
Reducing insulin resistance improves insulin receptor signaling at the cellular level. This allows glucose transport proteins to function correctly, enabling glucose to enter muscle and liver cells where it can be used for energy or stored as glycogen. This cellular-level correction is a defining feature of diabetes reversal.
As insulin sensitivity improves:
- Fasting blood glucose levels decline
- Post-meal glucose spikes are reduced
- Cellular energy utilization becomes more efficient
Scientific studies show that these improvements can occur early in the diabetes reversal process, often before major weight loss occurs.
3) Reduced Liver Insulin Resistance Normalizes Fasting Blood Sugar
The liver plays a dominant role in regulating fasting blood glucose by controlling glucose production and release. In insulin-resistant states, the liver becomes insensitive to insulin’s suppressive effects and releases glucose even when blood sugar levels are already elevated.
Reducing liver insulin resistance:
- Suppresses excessive hepatic glucose production
- Lowers fasting blood sugar levels
- Restores metabolic balance during overnight fasting
Research strongly links reductions in liver fat with improvements in hepatic insulin sensitivity, making liver health a cornerstone of diabetes reversal.
4) Improved Muscle Insulin Sensitivity Enhances Post-Meal Glucose Control
Skeletal muscle is the body’s largest glucose-absorbing tissue and is responsible for disposing of most glucose after meals. Insulin resistance in muscle tissue causes glucose to remain in circulation, leading to prolonged post-meal hyperglycemia.
When muscle insulin sensitivity improves:
- Glucose uptake increases significantly after eating
- Muscle glycogen storage capacity expands
- Blood sugar levels stabilize throughout the day
Scientific evidence consistently shows that improved muscle insulin sensitivity is essential for achieving and maintaining diabetes reversal.
5) Reduced Insulin Resistance Protects and Restores Pancreatic Function
As insulin resistance decreases, the pancreas no longer needs to produce excessive insulin to compensate. This reduction in insulin demand allows pancreatic beta cells to recover from chronic stress and dysfunction.
Research indicates that:
- Beta-cell exhaustion slows or reverses
- Insulin secretion becomes more responsive and efficient
- Long-term pancreatic function is preserved
Protecting beta-cell health is critical for sustaining diabetes reversal and preventing relapse.
6) Loss of Visceral Fat Improves Whole-Body Insulin Sensitivity
Visceral fat—fat stored deep in the abdominal cavity—releases free fatty acids and inflammatory compounds that directly interfere with insulin signaling. This makes visceral fat one of the strongest predictors of insulin resistance and type 2 diabetes.
Reducing visceral and ectopic fat:
- Improves insulin receptor signaling
- Decreases inflammatory stress on tissues
- Enhances whole-body insulin sensitivity
Research shows that even modest reductions in visceral fat can result in substantial improvements in blood sugar control and metabolic health.
7) Lower Inflammation Strengthens Insulin Signaling Pathways
Chronic low-grade inflammation disrupts insulin signaling at multiple points in the metabolic pathway. Inflammatory molecules impair insulin receptor function and block glucose transport mechanisms.
Reducing insulin resistance is associated with:
- Lower inflammatory markers
- Improved insulin signal transmission
- Enhanced glucose metabolism
Scientific studies consistently link reduced inflammation with improved insulin sensitivity and successful diabetes reversal.
8) Sustained Insulin Sensitivity Enables Long-Term Diabetes Reversal
Research emphasizes that diabetes reversal is not a one-time achievement but a sustained metabolic state. If insulin resistance returns, blood sugar levels can rise again.
Maintaining improved insulin sensitivity:
- Supports long-term blood sugar control
- Reduces medication dependence
- Promotes lasting metabolic health
Long-term studies show that individuals who maintain insulin sensitivity through lifestyle consistency are more likely to experience durable diabetes reversal.
What role does visceral fat play in diabetes reversal?

Visceral fat plays a critical role in both the development of type 2 diabetes and the process of diabetes reversal. Visceral fat refers to fat stored deep within the abdominal cavity, surrounding vital organs such as the liver, pancreas, and intestines.
Research consistently shows that excess visceral fat is metabolically active and strongly linked to insulin resistance, chronic inflammation, and poor blood sugar control. Reducing visceral fat is therefore one of the most powerful drivers of improving insulin sensitivity and achieving diabetes reversal.
Excess visceral fat disrupts normal metabolic function by releasing large amounts of free fatty acids directly into the portal circulation, which drains into the liver. This constant influx of fat interferes with insulin signaling and promotes excessive glucose production by the liver.
As visceral fat decreases, liver insulin sensitivity improves, leading to lower fasting blood sugar levels and more stable glucose regulation. This mechanism explains why reductions in visceral fat are closely associated with early improvements seen during diabetes reversal.
Visceral fat also plays a key role in worsening insulin resistance throughout the body. Unlike subcutaneous fat, visceral fat actively secretes inflammatory molecules that impair insulin receptor function in muscle, liver, and fat cells.
These inflammatory signals block glucose transport into cells, causing blood sugar to remain elevated. When visceral fat is reduced, inflammation decreases, insulin signaling improves, and glucose uptake becomes more efficient, key metabolic changes required for diabetes reversal.
Another critical aspect of visceral fat is its impact on pancreatic function. Fat accumulation around the pancreas interferes with insulin secretion by impairing beta-cell responsiveness.
Research shows that reducing pancreatic fat improves insulin release in response to glucose, restoring normal post-meal blood sugar control. This recovery of pancreatic function is a hallmark of sustained diabetes reversal.
Visceral fat is also closely linked to metabolic inflexibility, a condition in which the body struggles to switch between burning carbohydrates and fats efficiently. High visceral fat levels promote constant fat overflow into tissues, worsening insulin resistance and glucose dysregulation.
As visceral fat decreases, metabolic flexibility improves, allowing the body to regulate blood sugar more effectively across different metabolic states.
Key research-backed roles of visceral fat in diabetes reversal include:
- Drives insulin resistance in the liver, muscle, and fat tissue
- Increases hepatic glucose production, raising fasting blood sugar
- Promotes chronic inflammation that disrupts insulin signaling
- Impairs pancreatic beta-cell function and insulin secretion
- Worsens metabolic inflexibility and glucose instability
- Strongly predicts the likelihood of successful diabetes reversal
Overall, scientific research makes it clear that reducing visceral fat is central to diabetes reversal. By lowering insulin resistance, decreasing inflammation, restoring pancreatic function, and improving metabolic flexibility, loss of visceral fat allows the body to regain normal blood sugar control.
These improvements explain why interventions that specifically target visceral fat are consistently associated with lasting diabetes reversal and improved metabolic health.
How long does it take to see results from diabetes reversal strategies?

The timeline for seeing results from diabetes reversal strategies varies from person to person, but scientific research shows that meaningful improvements in blood sugar control, insulin sensitivity, and metabolic health can begin much sooner than many people expect.
The speed of results depends on factors such as diabetes duration, degree of insulin resistance, visceral fat levels, lifestyle consistency, and whether interventions are applied early. Below is a detailed, research-aligned breakdown of when different improvements typically occur.
1) Early Results: Days to 2 Weeks
Research shows that the earliest changes in diabetes reversal often occur within days to two weeks, particularly when dietary changes and calorie reduction are introduced. During this phase, improvements are driven primarily by reduced liver glucose production and improved hepatic insulin sensitivity, rather than weight loss.
Key early improvements include:
- Lower fasting blood sugar levels
- Reduced post-meal glucose spikes
- Decreased insulin demand
- Improved liver insulin sensitivity
Many individuals notice improved blood sugar readings within the first week, demonstrating that metabolic changes can begin rapidly.
2) Short-Term Results: 2 to 8 Weeks
Within two to eight weeks, more noticeable metabolic improvements typically occur. As insulin sensitivity improves across the liver and muscles, blood sugar control becomes more stable throughout the day. During this phase, modest weight loss and reductions in visceral fat begin to contribute more significantly to glucose regulation.
Common short-term results include:
- Improved insulin sensitivity
- More stable fasting and post-meal glucose levels
- Reduced need for glucose-lowering medication (under medical supervision)
- Decreased visceral fat and liver fat
This period often marks a turning point where diabetes reversal strategies start producing consistent, measurable results.
3) Medium-Term Results: 2 to 6 Months
Between two and six months, research shows that deeper metabolic changes occur. Continued lifestyle consistency leads to significant reductions in insulin resistance, improved muscle glucose uptake, and further reductions in liver and pancreatic fat.
At this stage, many individuals experience:
- Sustained normal or near-normal blood sugar levels
- Improved HbA1c readings
- Enhanced pancreatic beta-cell function
- Greater metabolic flexibility
Clinical studies show that individuals who maintain consistent diabetes reversal strategies during this phase have a higher likelihood of achieving diabetes remission.
4) Long-Term Results: 6 to 12 Months and Beyond
Long-term diabetes reversal results typically become evident after six to twelve months of sustained lifestyle changes. Research indicates that maintaining improved insulin sensitivity and reduced visceral fat over time allows normal glucose regulation to persist without medication in many individuals.
Long-term outcomes include:
- Stable blood sugar control without medication
- Durable improvements in insulin sensitivity
- Reduced risk of diabetes-related complications
- Improved overall metabolic health
Studies emphasize that long-term success depends on maintaining lifestyle changes that support insulin sensitivity.
5) Factors That Influence How Fast Results Appear
The speed of diabetes reversal varies based on several key factors:
- Duration of type 2 diabetes (earlier intervention leads to faster results)
- Baseline insulin resistance and visceral fat levels
- Dietary quality and calorie control
- Physical activity and muscle mass
- Sleep quality and stress management
- Consistency and adherence to lifestyle changes
Individuals with shorter diabetes duration and better-preserved pancreatic function tend to see faster and more durable results.
6) Why Diabetes Reversal Timelines Differ Between Individuals
Research shows that diabetes is a progressive metabolic condition, and reversal strategies work by correcting long-standing dysfunctions. For some, improvements occur rapidly; for others, progress is gradual but steady. What matters most is sustained improvement in insulin sensitivity rather than rapid short-term changes.
Who can benefit most from diabetes reversal approaches?

People who benefit most from diabetes reversal approaches are those whose metabolic dysfunction is still responsive to improvements in insulin sensitivity, body fat distribution, and lifestyle change.
Research shows that diabetes reversal is most achievable in individuals with type 2 diabetes or prediabetes, particularly when interventions are applied early and consistently. While results vary, certain metabolic and clinical characteristics strongly predict better outcomes.
Individuals with prediabetes are among the most responsive to diabetes reversal strategies because insulin resistance and beta-cell dysfunction are still relatively mild.
In this stage, blood sugar levels can often return to normal with targeted changes in nutrition, physical activity, weight management, sleep quality, and stress reduction. Research indicates that early intervention at the prediabetes stage significantly lowers the risk of progressing to type 2 diabetes and improves long-term metabolic health.
People with recently diagnosed type 2 diabetes also benefit greatly from diabetes reversal approaches. Studies show that individuals with a shorter duration of diabetes tend to have better-preserved pancreatic beta-cell function, making it easier to restore normal insulin secretion and blood sugar control.
In these cases, reducing insulin resistance and visceral fat can lead to sustained improvements and, in some individuals, diabetes remission without medication under medical supervision.Those with significant insulin resistance and excess visceral fat often experience pronounced benefits from diabetes reversal strategies.
Visceral fat is strongly linked to insulin resistance, chronic inflammation, and poor glucose regulation. Research demonstrates that individuals who reduce visceral fat particularly liver and pancreatic fat show rapid improvements in insulin sensitivity and fasting blood sugar levels, making them strong candidates for diabetes reversal.
Individuals who are overweight or obese, especially with abdominal fat accumulation, tend to respond well to diabetes reversal approaches because weight loss and improved body composition directly reduce insulin resistance.
Even modest weight loss has been shown to produce significant metabolic benefits, including improved blood sugar control and reduced insulin demand.
People who are motivated and able to maintain lifestyle changes benefit the most over the long term. Diabetes reversal is not a one-time intervention but a sustained metabolic state.
Research consistently shows that individuals who can adhere to dietary improvements, regular physical activity, adequate sleep, and stress management achieve more durable results and lower relapse risk.
Key groups who benefit most from diabetes reversal approaches include:
- Individuals with prediabetes
- People with early or recently diagnosed type 2 diabetes
- Those with high insulin resistance
- Individuals with excess visceral or abdominal fat
- People who are overweight or obese
- Individuals with preserved pancreatic beta-cell function
- Those willing to commit to long-term lifestyle changes
Overall, research indicates that diabetes reversal approaches are most effective when applied early, targeted toward improving insulin sensitivity, and sustained over time. People who meet these criteria are more likely to achieve lasting improvements in blood sugar control and overall metabolic health.
If you’re inspired by the science behind diabetes reversal and want to take actionable steps toward lasting blood sugar control, the right guidance can make all the difference. The Healthywayfit program is designed to help you apply evidence-based nutrition, exercise, and lifestyle strategies in a structured, sustainable way.
With personalized support, clear plans, and expert tips, Healthywayfit empowers you to improve insulin sensitivity, reduce visceral fat, and achieve real, long-term results turning the concept of diabetes reversal into a practical, achievable reality.
HealthyWayFit — India’s Most Personal Diabetes Reversal Program

You’re told to “eat less,” “exercise more,” or “try another pill.” Yet your sugars remain stubborn, energy crashes continue, and every lab report feels like another warning. What’s missing isn’t willpower — it’s the right system.
That’s where HealthyWayFit comes in.
We are not another app, crash diet, or one-size-fits-all chart. HealthyWayFit is a 12-month, end-to-end Type 2 Diabetes Reversal Program designed exclusively for Indian professionals who want results that fit their lifestyle.
Over the past few years, our team has helped hundreds of Indians lower HbA1c, reduce medicine dependency, and—in many cases—achieve complete reversal of Type 2 diabetes.
Our tone is simple: empathetic, therapeutic, and committed. We listen first, design second, and support you every step of the way.
1) What Makes HealthyWayFit Different?
1. Personalized Nutrition You Can Actually Follow No fad superfoods or unrealistic smoothie charts. We use your ghar ka khana—dal, roti, rice, idli, dosa, paneer, sabzi—and align it with blood sugar control. No separate cooking, no family pressure. A plan that works whether you’re 35 or 85.
2. Metabolic Exercise for Type 2 Diabetes Control Our short, 15–20 minute metabolic routines target big muscle groups (legs, shoulders, glutes) and can lower sugar readings by 50–100 points. No gym, no equipment, just science-backed movements you can do at home.
3. Stress & Sleep Mastery Stress raises cortisol, which raises sugar. We equip you with practical tools—one-minute breathing practices, sleep optimization, and micro-habits—to keep your blood sugar stable, even on your busiest days.
4. Doctor-Led, Holistic Care Every client is guided by a Senior MD Diabetologist ensuring medical safety, while lifestyle coaches design food, exercise, and habit strategies. This unique blend of medical expertise and daily support is why our clients see true reversal.
5. Relentless Support & Accountability From weekly coaching calls and daily check-ins to festival, travel, and dining-out guides, we make sure your reversal journey adapts to real life, not the other way around.
2) What Results Can You Expect?
Most clients notice changes within 20–60 days: better energy, lighter mornings, and lower sugar readings. Over the year, we focus on long-term stabilization, so results are not just quick but sustainable for years to come.
3) Is HealthyWayFit Right for You?
If you’re a working professional or entrepreneur living with Type 2 diabetes, and can dedicate just 15–30 minutes daily, HealthyWayFit is built for you. This isn’t a crash course. It’s a life-changing reversal system personalized to your food, family, and lifestyle.
4) Take the Next Step
Your journey starts with a personal consultation where we understand your health history, challenges, and lifestyle. If we’re aligned, we’ll design a custom Type 2 Diabetes Reversal Plan built just for you.
Explore more at: healthywayfit Book your consultation here: calendly
Move beyond “managing” diabetes. With HealthyWayFit, you can reverse Type 2 diabetes—safely, sustainably, and with support at every step.
Frequently Asked Questions (FAQs)

1) Can diabetes reversal lead to lasting results?
Yes, diabetes reversal can lead to lasting results when the underlying causes especially insulin resistance, excess visceral fat, and poor metabolic health are addressed and maintained.
Research shows that individuals who sustain healthy lifestyle changes such as balanced nutrition, regular physical activity, weight management, adequate sleep, and stress control can maintain normal blood sugar levels for years. Long-term success depends on consistency, as returning to insulin-resistant habits can cause blood sugar levels to rise again.
2) What lifestyle factors are essential for sustaining diabetes reversal?
Sustaining diabetes reversal requires lifestyle factors that continuously support insulin sensitivity and metabolic health. These include a nutrient-dense, whole-food diet, regular physical activity combining aerobic and resistance training, maintaining a healthy body weight, prioritizing quality sleep, managing chronic stress, and limiting ultra-processed foods.
Consistency across these factors helps prevent the return of insulin resistance and supports stable, long-term blood sugar control.
3) Is diabetes reversal permanent if blood sugar normalizes?
Diabetes reversal is not considered permanent in a biological sense, even if blood sugar normalizes. Research shows that normal glucose levels can be maintained long term, but only as long as the metabolic improvements that enabled reversal are preserved.
If insulin resistance returns due to weight gain, inactivity, or poor diet, blood sugar levels can rise again. Ongoing lifestyle management is essential to sustain results.
4) What is the difference between diabetes reversal and diabetes remission?
Diabetes reversal is a broader, non-clinical term describing improved blood sugar control through lifestyle changes without medication. Diabetes remission is a clinical term used in research and medical guidelines, defined as maintaining normal blood sugar levels for a specific period without glucose-lowering drugs.
Both describe similar outcomes, but remission is a formally measured medical state, while reversal emphasizes the process and lifestyle-driven improvement.
5) Does diabetes reversal work for both prediabetes and type 2 diabetes?
Yes, diabetes reversal approaches can work for both prediabetes and type 2 diabetes, though outcomes differ. Individuals with prediabetes often experience faster and more complete normalization of blood sugar because insulin resistance and beta-cell damage are less advanced.
People with type 2 diabetes can also achieve reversal or remission, especially when diagnosed early and when lifestyle changes are applied consistently and sustained over time.
Conclusion
In conclusion, diabetes reversal is a scientifically supported, achievable process that goes far beyond simply lowering blood sugar. By addressing the root causes of type 2 diabetes particularly insulin resistance, excess visceral fat, and metabolic dysfunction research shows that blood sugar can return to a non-diabetic range, often without the need for medication.
Key strategies such as improving insulin sensitivity, reducing liver and pancreatic fat, adopting a nutrient-dense diet, engaging in regular physical activity, and managing stress and sleep are central to achieving and sustaining lasting results. While the timeline and degree of reversal vary between individuals, early intervention and consistent lifestyle changes greatly increase success rates.
Importantly, diabetes reversal is a long-term commitment rather than a quick fix, requiring ongoing adherence to healthy habits. Programs like HealthyWayFit provide structured guidance, personalized plans, and continuous support, making it possible to turn the concept of diabetes reversal into a practical, real-world solution for lasting metabolic health.

